- Home
- Conditions and Care
- Conditions
- Spider Veins
Spider Veins
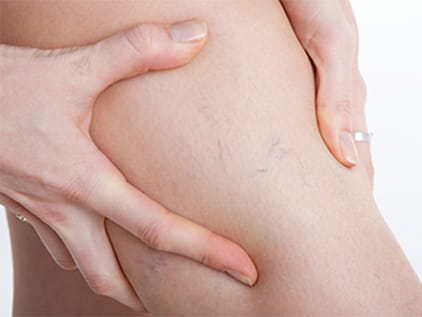
Spider veins are small, thin veins that lie close to the surface of the skin, appearing as clusters of red, blue or purple veins. Technically a mild form of varicose veins, spider veins can cause symptoms that range from mild discomfort, burning and itching, despite their smaller size.
At The University of Kansas Health System, our specialists provide a variety of options for spider vein treatment. They'll work with you to determine the best course of treatment based on the size, location and severity of your spider veins.
What are spider veins?
Spider veins are small, fine, varicose veins within the skin. Although spider veins are commonly found on the thighs, calves, ankles and feet, they can also be found on the face. They can cover either a very small or very large area of skin.
Spider veins may take on 1 of 3 basic patterns:
- Linear, appearing as thin separate lines
- Tiny branch-like shapes
- True spider shape, with a group of veins radiating outward from a dark central point
Spider veins cannot always be prevented. Wearing support hose may minimize unwanted blood vessels from developing. Weight control and regular exercise may be helpful. Sun protection is important to limit the number of unwanted vessels on the face.
We offer a variety of appointment types. Learn more or call 913-588-1227 to schedule now.
Spider vein symptoms and risks
For some, spider veins have no symptoms and may be mainly a cosmetic concern. However, other people can experience aching, burning, itching and, in rare cases, bleeding from their spider veins.
The cause of spider veins is not completely known, although they often run in families. There are many factors that can contribute to getting spider veins:
- Heredity
- Occupations or activities that require prolonged sitting or standing
- Other events that cause hormonal shifts
- Pregnancy
In fair-skinned people, spider veins on the nose and the cheeks can also be related to sun exposure. Spider veins can appear in both men and women, but are seen more frequently in women.
Spider vein diagnosis and screening
Your doctor can usually diagnose spider veins by sight during a physical exam. In some cases, your doctor may recommend additional testing to determine or rule out possible underlying causes for your spider veins, or to screen for other types of vascular disease.
Injections for spider veins
Sclerotherapy is a minimally invasive treatment for people with spider veins. This procedure shrinks blood vessels to improve your appearance and reduce related vascular symptoms.
Spider vein treatment
Not all spider veins require treatment, and there are several lifestyle changes that may help prevent the formation of spider veins and varicose veins:
- Avoid standing for long periods.
- Use of compression stockings.
- Elevate your legs when resting.
- Exercise regularly.
- Maintain a healthy weight.
If you already have spider veins in your legs, compression socks may help you feel more comfortable.
For spider veins that do require treatment, The University of Kansas Health System offers multiple vein treatments. The most common treatment option for spider veins is sclerotherapy. During sclerotherapy, a special solution is injected directly into the blood vessel with a fine needle. The solution irritates the lining of the vessel, causing it to swell and stick together, and causing the blood to clot. Over several weeks, the vessel turns into scar tissue and eventually fades, becoming barely noticeable.
A single blood vessel may have to be injected more than once, usually weeks to months apart, depending upon its size. A number of vessels may be injected at any treatment session. After several treatments, most people can expect significant improvement. Fading of the spider veins occurs gradually over a period of months.

Still the best
Our hospital continues to rank as the best in Kansas City and in Kansas according to U.S. News & World Report.

Magnet-recognized
The University of Kansas Hospital has been designated a Magnet® facility by the American Nurses Credentialing Center since 2006. 
Respect for all people
Established inclusive practices through our work with the Human Rights Campaign. 



