Our World-Class Services

At The University of Kansas Health System, we harness the latest medical advancements to deliver innovative treatments that transform lives. From proton therapy to our lifesaving brain and neurological care, we ensure every patient receives world-class treatment for even the most complex conditions.
Our world-class National Cancer Institute-designated comprehensive cancer center is one of fewer than 60 nationwide. Only institutions demonstrating scientific excellence through a rigorous peer review process receive NCI designation. As a result, our patients have better access to clinical trials, the latest therapies and more personalized care closer to home.
We treat patients with breast, lung, prostate, sarcoma, colon, and head and neck cancers, offering increased patient access to world-renowned experts and world-class care. We also offer the region's largest blood and marrow transplant program for the treatment of complex blood cancers like leukemia and lymphoma.

The Proton Therapy Center at The University of Kansas Cancer Center is the only one of its kind in the region. The University of Kansas Cancer Center is a National Cancer Institute-designated comprehensive cancer center – 1 of fewer than 60 NCI comprehensive centers in the nation and the only NCI center in the region.
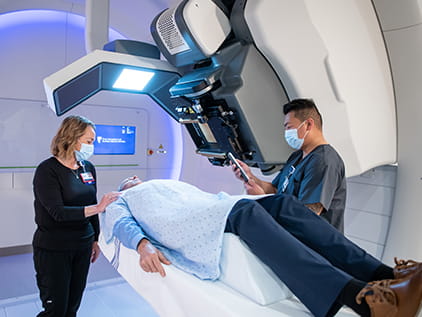
When you choose The University of Kansas Cancer Center for proton therapy treatment, your patient will receive personalized, precision medicine from a multidisciplinary team of experts in cancer care.
Our comprehensive approach to prostate cancer care includes the most innovative treatment options. Along with providing these advanced treatments, our physicians lead national and international clinical trials for early-stage, advanced and metastatic prostate cancer. Learn more about our nationally ranked urology program and exceptional level of knowledge, expertise and multidisciplinary care.

Nationally renowned specialists at the Center for Advanced Brain and Neurological Care provide expert diagnoses and treatment for complex disorders affecting the brain, spinal cord and nervous system. These include stroke, brain aneurysms, tumors and traumatic brain injury, as well as conditions such as epilepsy and Parkinson's disease.
Our health system was 1 of the first 4 in the nation and the first in Kansas City recognized as an Advanced Comprehensive Stroke Center by The Joint Commission.
Spine specialists and surgeons at our Marc A. Asher, MD, Comprehensive Spine Center provide complex diagnoses and the best treatment options for conditions, including degenerative disc disease, herniated disc and spinal cord tumors.

Our doctors and surgeons at the Sports Medicine and Performance Center specialize in the prevention of sports injuries and disorders, improving health with advanced surgical and nonsurgical care. We are the official healthcare provider of the Kansas City Chiefs, Kansas City Royals and T-Mobile Center.

The health system is home to the region’s only nationally verified Level I Trauma Center. We provide 24/7 on-site treatment for time-critical diagnoses, including STEMI, stroke, burns, 24/7 acute leukemia and other critical conditions. Our board-certified specialists include trauma surgeons, emergency medicine physicians, neurosurgeons, orthopedists, plastic surgeons, radiologists and nurses, providing a full spectrum of emergency care.
Our burn center is the only burn center in the region accredited for both adult and pediatric burns by the American Burn Association and the American College of Surgeons. Patients receive individualized care for complex burns and wounds, and support and resources to increase comfort and speed recovery.

The Women’s Cancer Center at The University of Kansas Cancer Center focuses exclusively on breast and gynecologic cancers. As the only National Cancer Institute (NCI)-designated comprehensive cancer center in the region, The University of Kansas Cancer Center offers more clinical trials and more treatment options.
The Women’s Cancer Center provides integrated, multidisciplinary care with a patient-centric approach for the most common cancers in women. Our team of academic experts comprises numerous female cancer specialties, including breast and gynecologic surgical oncology, breast medical oncology and breast reconstruction and plastic surgery.
Learn more about The Women’s Cancer Center.

We have one of the most comprehensive cardiology and heart surgery programs in the region and provide the full spectrum of cardiovascular services. Our advanced heart failure and transplant program includes a multidisciplinary team comprising cardiologists, cardiothoracic surgeons, cardiac nurse navigators and other professionals. These specialists work together, share information and identify the best possible course of treatment for each patient.
Our nationally recognized heart care program offers innovative treatments, sees lower readmission rates and a shorter length of stay for patients. It is the first heart program in the nation to receive Comprehensive Cardiac Center certification from The Joint Commission.

Specialty areas
From maternal-fetal medicine to solid organ transplant, our specialists address the most complex conditions.




