- Home
- Conditions and Care
- Conditions
- Moyamoya Disease
Moyamoya Disease
Our specialty-trained neurosurgeons are among few in the region skilled at diagnosing and treating moyamoya disease. The condition name means “puff of smoke” in Japanese, a name that comes from the appearance of the cluster of tiny blood vessels that signify the disease. Our team has treated hundreds of people for moyamoya disease.
At The University of Kansas Health System in Kansas City, we offer unparalleled experience recognizing and correcting this unusual and dangerous condition.
What is moyamoya disease?
Moyamoya disease is a rare blood vessel disorder. It is a condition that occurs when the walls of the carotid artery in the skull thicken, reducing blood flow to the brain. In response, tiny blood vessels open at the base of the brain to try to compensate for the blocked artery. These tiny vessels cannot fully supply the blood the brain needs, which increases the risk for transient ischemic attacks (TIA), stroke or aneurysm.
Moyamoya disease can lead to temporary or permanent brain damage and can be fatal if unrecognized and untreated.
We offer a variety of appointment types. Learn more or call 913-588-1227 to schedule now.
Moyamoya disease symptoms and risks
The symptoms of moyamoya disease are those that occur when reduced blood flow to the brain decreases the brain's oxygen supply:
- Cognitive decline
- Developmental delays in children
- Headache
- Seizures
- Speech difficulties, or difficulty understanding others (aphasia)
- Visual disturbances
- Weakness, numbness or paralysis in the face, arm or leg, often on just one side of the body
Several of the signs of moyamoya disease are similar to those of stroke. If you think you or someone you know may be experiencing moyamoya disease or stroke, contact your doctor immediately.
Moyamoya disease most often affects children ages 5-10 but can affect anyone. In adults, the typical onset age is between 30-50 years old. Occurring in women slightly more often than men, moyamoya disease is most commonly found in East Asian countries, such as Korea, Japan and China, and in people of East Asian descent.
Moyamoya disease diagnosis and screening
To diagnose moyamoya disease, your doctors will begin with a full physical exam and discussion of your medical history and your family history. Doctors may also schedule a variety of imaging studies – such as MRI, CT scan or PET scan – to create detailed pictures of your brain.
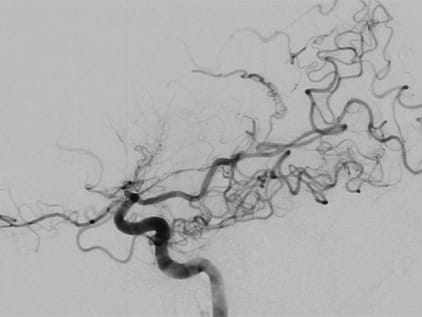
One study that is helpful in diagnosis of moyamoya disease is the cerebral angiogram. This is a test in which dye is injected into your brain to help doctors visualize the blood flowing to the brain. The images will show any blockage and also will allow the doctors to see the cluster of tiny blood vessels at the base of the brain that is the telltale sign of moyamoya disease.
From operating room to emergency room
Surgical technologist Jason Edwards was working in the operating room when his arm went limp. Tests confirmed he suffered a ministroke caused by moyamoya disease.
Moyamoya disease treatment
Medication such as blood thinners or antiseizure medications may be part of your treatment plan, but most people with moyamoya disease require surgery for lasting results. Your neurosurgeon may perform direct or indirect surgical correction.
Doctors choose the direct method for adults with moyamoya disease when an immediate improvement in blood flow to the brain is necessary to avoid further and potentially permanent brain damage.
Why choose us for moyamoya disease care?
Our neurosciences program is the region's largest, and U.S. News & World Report has consistently ranked our neurology and neurosurgery services among the nation's top 50. Survival rates, patient safety and specialized staff all contribute to this success.
Our neurosurgeons are fellowship-trained and our neurology care team has unparalleled experience in treating moyamoya.

Find a doctor
Doctors at The University of Kansas Health System are care providers and researchers at the forefront of new medical discoveries. From primary care to complex conditions, we offer hundreds of specialists.




